Vanuatu Ministry of Health piloted an MDA campaign targeting several NTDs, with skin exams and referral to the primary health care system, and also conducted surveillance for multiple disease targets.
A South Pacific Ocean nation made up of roughly 13 principle islands and many more smaller islands that stretch across 800+ miles.
As part of a larger implementation project, the Vanuatu Ministry of Health (MoH) piloted integrating an MDA campaign targeting yaws, scabies, and soil-transmitted helminths (STH), with skin exams and referral to the primary health care system. In addition, in a subset of villages, the project also integrated the collection of dried blood spots (DBS) for multi-disease serosurveillance and stool samples to assess prevalence of STH.
Bridges to Development conducted research to evaluate the feasibility of the fully integrated campaign including: multi diseases MDA; skin examinations and referral to the primary health care system for further treatment; and sample collection for serosurveillance and monitoring and evaluation (M&E).

Vanuatu is one of the first countries to eliminate lymphatic filariasis with a strong national and provincial capacity to implement community outreach activities. A highly committed NTD team is working on the elimination of yaws and leprosy & control of scabies and soil-transmitted helminths. They have submitted their dossier to the WHO to validate the elimination of trachoma as a public health problem.
Tafea province, the site of our project, is the southernmost of the six provinces, with a population of 36,799 people, consisting of 5 islands, some of which are among the most isolated in Vanuatu.
As a part of a larger implementation project, the Vanuatu Ministry of Health (MoH) piloted a new integrated MDA approach in the Tafea Province:
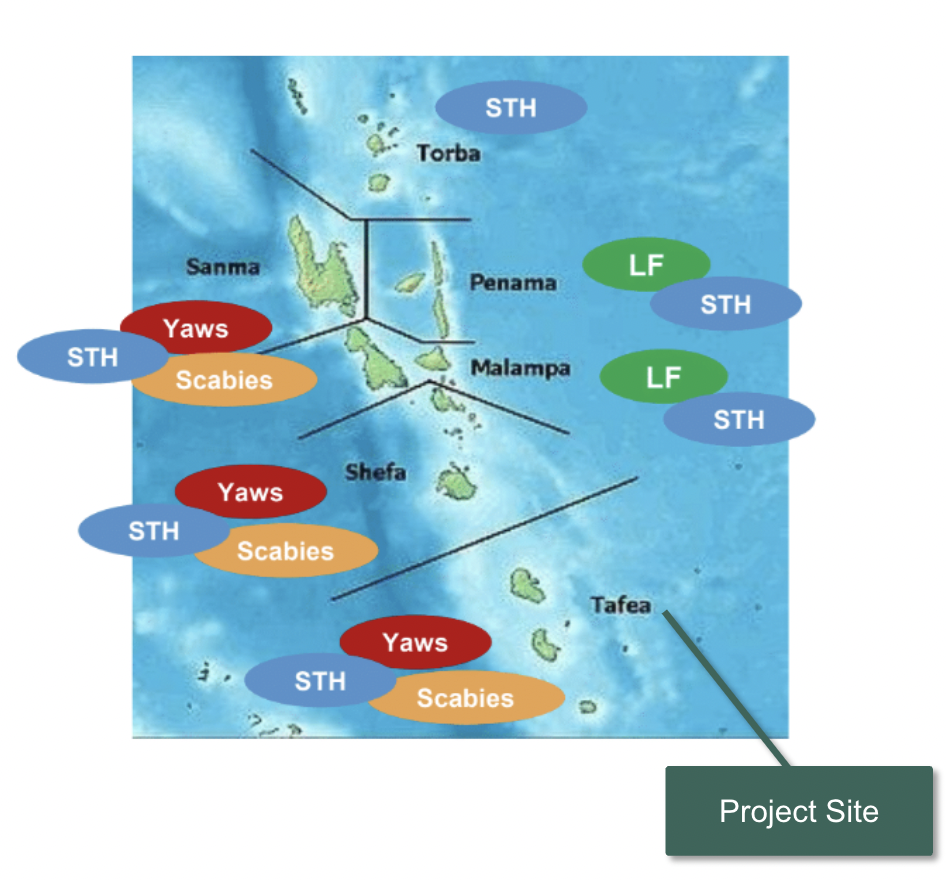
Image above: Map of Vanuatu and where specific NTDs are prevalent.

Table above: NTDs and the associated goals for the study in Vanuatu.
Of a total population of 36,799 people, 26,895 people participated and were treated in the MDA campaign yielding an overall coverage of 73%; the WHO and country target were 80%. As part of the registration process, 7,212 people self-reported suspected yaws, leprosy or other severe skin disease and were referred to and examined by a nurse. Upon examination by a nurse, 342 people were clinically confirmed as having a severe skin disease and received a referral form to visit a primary health care center for follow up care. During this process, 164 suspected cases of yaws were identified with 12 confirmed with the DPP assay. As part of the monitoring and evaluation activities, 243 DBS were collected out of a target of 293 (83% of target). However, only 149 out of a target of 731 stool samples were collected (20% of target) demonstrating a higher resistance from the community to providing stool samples. Despite the low number of samples collected, STH prevalence was determined to be quite high in the communities: 46.9% for ascariasis; 43.4% for trichuriasis; and 25.2% for hookworm.
Anastasia Pantelias, Bridges to Development, walks through the objectives, methods, lessons and policy implications.
The field team in Vanuatu was composed of 84 health workers and volunteers. Thirty-one (36.90%) of those participated in the feasibility survey. When asked if they agreed with the statement that conducting skin exams in the community and referring cases of severe diseases to the health centers for care is a valuable health service for the community, 100% of respondents either agreed (50%) or strongly agreed (50%). Furthermore, 66.7% of respondents strongly agreed and 33.3% agreed that integrating skin exams and referral with the MDA campaign is a valuable health service to the community. Participants commented that it is valuable as it allows “to identify an early outbreak and treat immediately”, “Treatment on the spot”, “Improve community lifestyle, prevent further complications and restore confidence between nurses and community”, “Save lives and prevent community transmission”, “to reduce diseases.”
The majority of health workers agreed that the training on skin diseases helped them understand when a community member should be referred to the health center for additional care for a skin lesion. However, 22% of health workers did not feel prepared to evaluate which community members should be referred to the health center for additional care or follow up, and 11.1% did not feel prepared to perform skin exams. Questions were also asked about feasibility and community concern of the dry blood and stool collection that happened during the MDA campaign. It was reported that 60% of the professionals in charge of the stool collection found it difficult, while 20% found it very difficult. Furthermore, 80% of respondents believed community members were concerned about providing stool samples, mainly due to cultural barriers.

Reflecting on lessons learned and feedback received from participants in the feasibility survey, these promising practices were developed and should be pursued in future health campaigns and integration research.
In addition, see the research brief for lessons learned and implications for policy and future research.